Multimorbidity (≥2 chronic conditions per individual) is considered to be the most common chronic condition1 and a prevalent problem in primary care.2 In Portugal, citizens are covered by a national primary care network of public health centres,3 that play a gatekeeper role; a similar situation is found in Spain.
Despite the high accessibility of the public primary care sector, the number of health-insured people is growing. In Portugal, 2.2 million had health insurance in 2008.4
Since population ageing is a major force for higher prevalence estimates of multimorbidity and at the same time for an increase of the demand for primary care services, one could hypothesize that the private sector in primary health care will feel the same multimorbidity related pressures of the public sector.
To test this assumption, a cross-sectional descriptive study was performed in the Centre Region of Portugal during 2015. The aim was to characterize the profile of the private health care sector users and to compare their multimorbidity to the one found in a previously published Portuguese primary care study conducted in the public sector.5
Participants were 110 adult patients (63 women and 47 men) listed in a single-centre in the private sector. All listed patients were included. This health unit was chosen because of the similarities to the public sector's health centres: high accessibility (no appointment required), open every day for extended hours and provides ambulatory medical care to adults and children for low-acuity conditions. Sociodemographic and clinical variables were collected through the assessment of medical files and coded in the same way as the previously published public sector study data (Table 1).
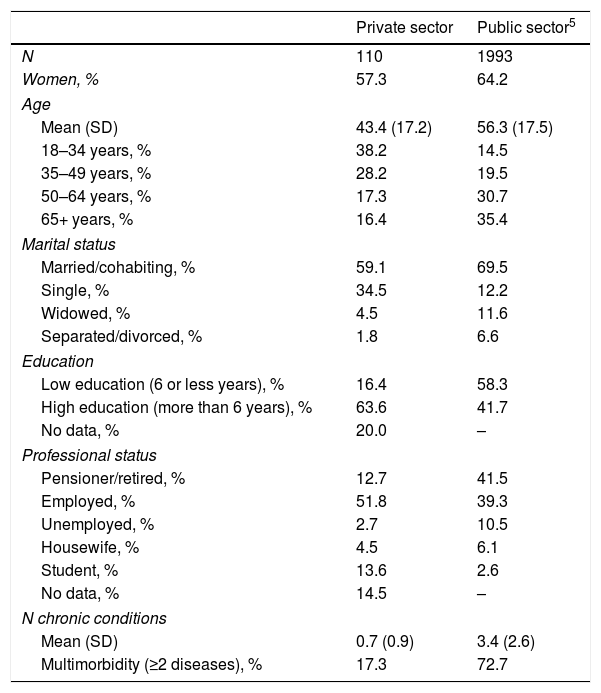
Characteristics of private and public sectors population samples.
| Private sector | Public sector5 | |
|---|---|---|
| N | 110 | 1993 |
| Women, % | 57.3 | 64.2 |
| Age | ||
| Mean (SD) | 43.4 (17.2) | 56.3 (17.5) |
| 18–34 years, % | 38.2 | 14.5 |
| 35–49 years, % | 28.2 | 19.5 |
| 50–64 years, % | 17.3 | 30.7 |
| 65+ years, % | 16.4 | 35.4 |
| Marital status | ||
| Married/cohabiting, % | 59.1 | 69.5 |
| Single, % | 34.5 | 12.2 |
| Widowed, % | 4.5 | 11.6 |
| Separated/divorced, % | 1.8 | 6.6 |
| Education | ||
| Low education (6 or less years), % | 16.4 | 58.3 |
| High education (more than 6 years), % | 63.6 | 41.7 |
| No data, % | 20.0 | – |
| Professional status | ||
| Pensioner/retired, % | 12.7 | 41.5 |
| Employed, % | 51.8 | 39.3 |
| Unemployed, % | 2.7 | 10.5 |
| Housewife, % | 4.5 | 6.1 |
| Student, % | 13.6 | 2.6 |
| No data, % | 14.5 | – |
| N chronic conditions | ||
| Mean (SD) | 0.7 (0.9) | 3.4 (2.6) |
| Multimorbidity (≥2 diseases), % | 17.3 | 72.7 |
The main private sector user profile was different to the one described for the public sector.
The most common private health care sector user was female, around 43 years old, married, employed and with a high educational level. About 17% of the patients were multimorbid. Twenty-four patients (21.8%) presented hypertension, 16.4% depression, 10.9% persistent rhinitis, 9.2% dyslipidaemia, and 6.4% were obese.
The public sector user was in average older, had a lower educational level and was a pensioner/retiree. Was also more multimorbid (mean of 3.4 chronic conditions per patient versus 0.7 conditions in the private sector). These differences may be explained by: (i) generally there is no new health insurance subscriptions for individuals over the age of 60,4 so they have no choice but to use the public sector, and (ii) older patients have in average more chronic and complex conditions, and consequently may be more inclined to seek referral to a specialist through the public sector. North American literature6 is consistent with the current study results. Private health sector is mostly used by younger adults and the majority do not have a primary care physician.6
The main limitation of this study is that the results appear difficult to compare. The private sector sample is small, from only one health unit, and may not be generalizable nationwide. Further studies are required with larger samples.
From the current study, one can realize that presently the management of multimorbidity is mainly a public sector endeavour. Nonetheless, the number of 65+ year olds that visit healthcare providers in the private sector is increasing.6 In the future, the reality of chronic conditions’ management may change.