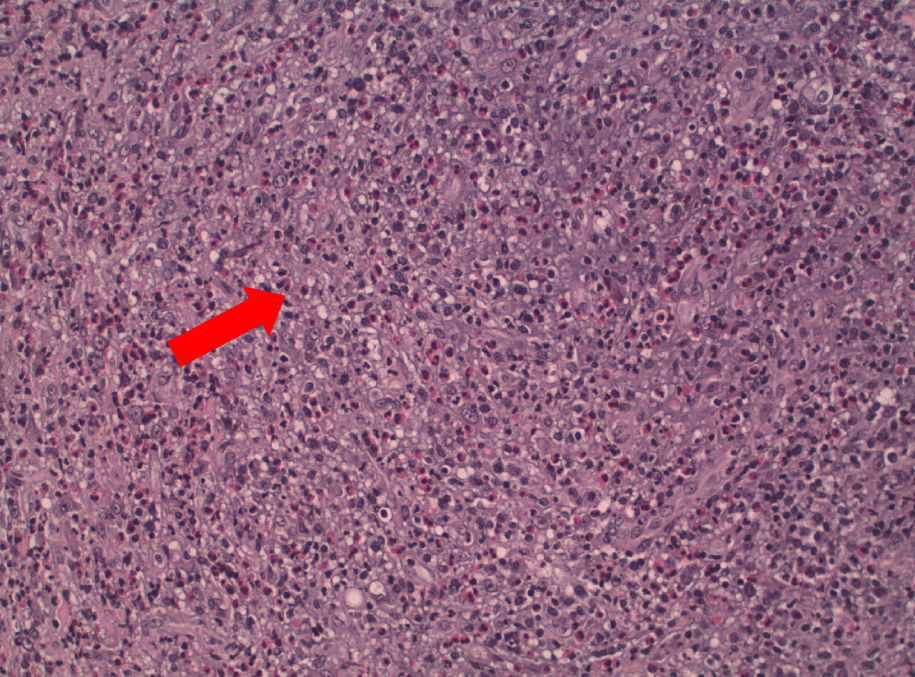
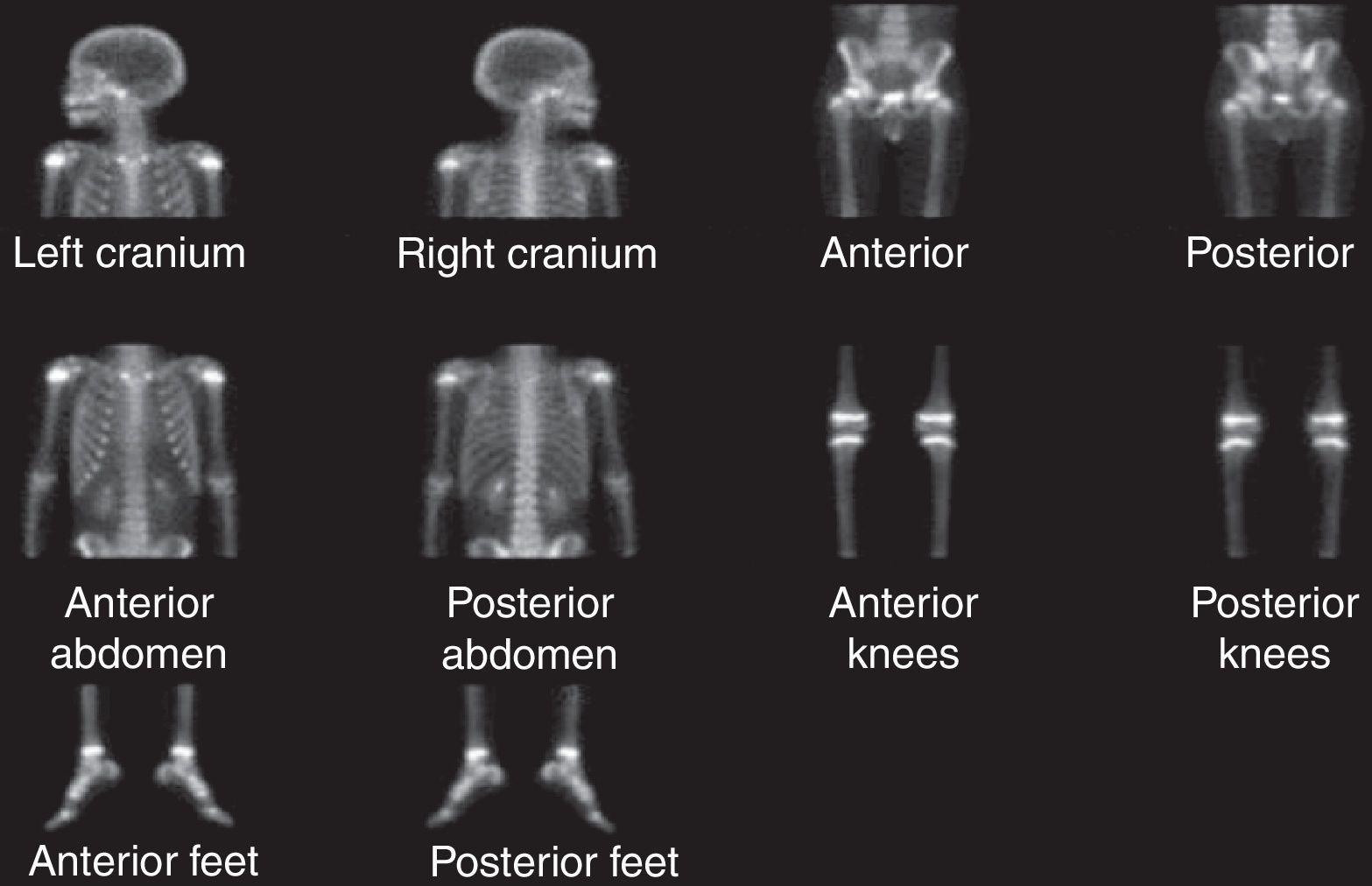
Anaplastic large T-cell lymphoma is a very rare disease in childhood. The most common locations are lymph nodes and skin, while the external ear location is uncommon. We present the case of a 6-year-old child with an earlobe tumour. Surgical treatment was performed and the anatomopathological results showed anaplastic large cell lymphoma. Radiological tests were negative and there was no systemic involvement.
El linfoma anaplásico de células grandes es una patología rara en la infancia. La localización más frecuente es en la piel y nódulos linfáticos, siendo infrecuente la afectación del pabellón auricular. Presentamos el caso de un niño de 6 años con tumoración en el lóbulo de la oreja. Se realizó tratamiento quirúrgico y el resultado de la anatomía patológica mostró linfoma anaplásico de células grandes. Los estudios radiológicos fueron negativos y no hubo afectación sistémica.